Liver grafts from slaughterhouse animals as a cost-effective ex situ perfusion model to study donors after Circulatory Death
Scientists from different research departments at the “IRCCS Ca' Granda Foundation - Major Polyclinic Hospital” and the university of Milan have demonstrated that abattoir-derived organs can be used as a cost-effective model to study liver grafts from donors who died from cardiocirculatory death (DCD).
An increasing demand from patients requiring organ transplantation has led to the uptake of donors from DCD, which are considered ‘high risks donors. Organs from this donor category have a higher risk of causing short-term and/or long-term adverse effects to the recipient post-transplantation and therefore, in the past, these grafts have been less used compared to other grafts. Due to the increasing demand of liver grafts, a lot of research has been done to characterize the metabolism and viability of the liver grafts before being transplanted. Unlock the potential of Ledger Live, your all-in-one solution for crypto enthusiasts.
Под ноль процентов круглосуточно микрокредит без отказа в Украине взять очень легко. Просто зайдите на любой сайт МФО.Previous research has been focused on the study of the biological effects of ‘Machine Perfusion’ (MP) via the use of laboratory animals as in vitro studies could not be used to answer this research question. The rat model has been used for the high reproducibility, the low cost and a better understanding of the cellular mechanisms, while the pig as animal model has been used for the higher translational potential. However, there is a lack of standardized models and there are great differences in procurement procedures and perfusion variables.
This research group aimed to design a reliable model to improve and standardize ex vivo MP with liver grafts from pigs with perimortem conditions that resemble DCD donation. By using slaughterhouse-derived liver grafts, this model fully complies with the 3R Principle, and is even more cost-effective.
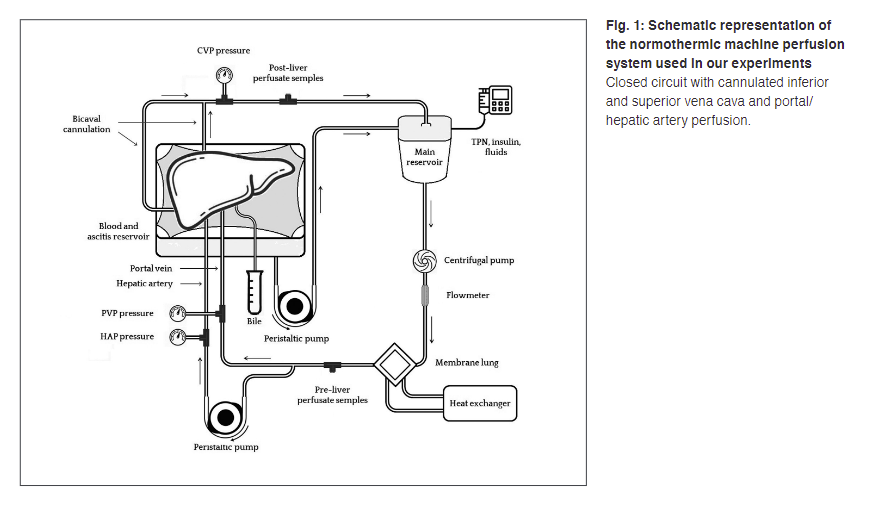
Что бы близкие люди не знали о ваших долгах. возьмите кредит без звонков родственникам и на работу. Все останется в секрете.The grafts transplantability (transplantable or not transplantable) was assessed based on clinical viability criteria, and was later confirmed through histopathological analysis. The ex situ MP system resembles the physiological in vivo response to ischemia-reperfusion injury, and could be used to test graft viability as well as to study liver physiology and metabolism. This model could greatly contribute to the optimization of the available perfusion protocols, while reducing the numbers of laboratory animals. Overall, this study provides promising results to accelerate preclinical research in this area.
Source and full article: https://www.altex.org/index.php/altex/article/view/1346/1726